Sodium vs Potassium: What’s the Difference & Which One Do You Need?
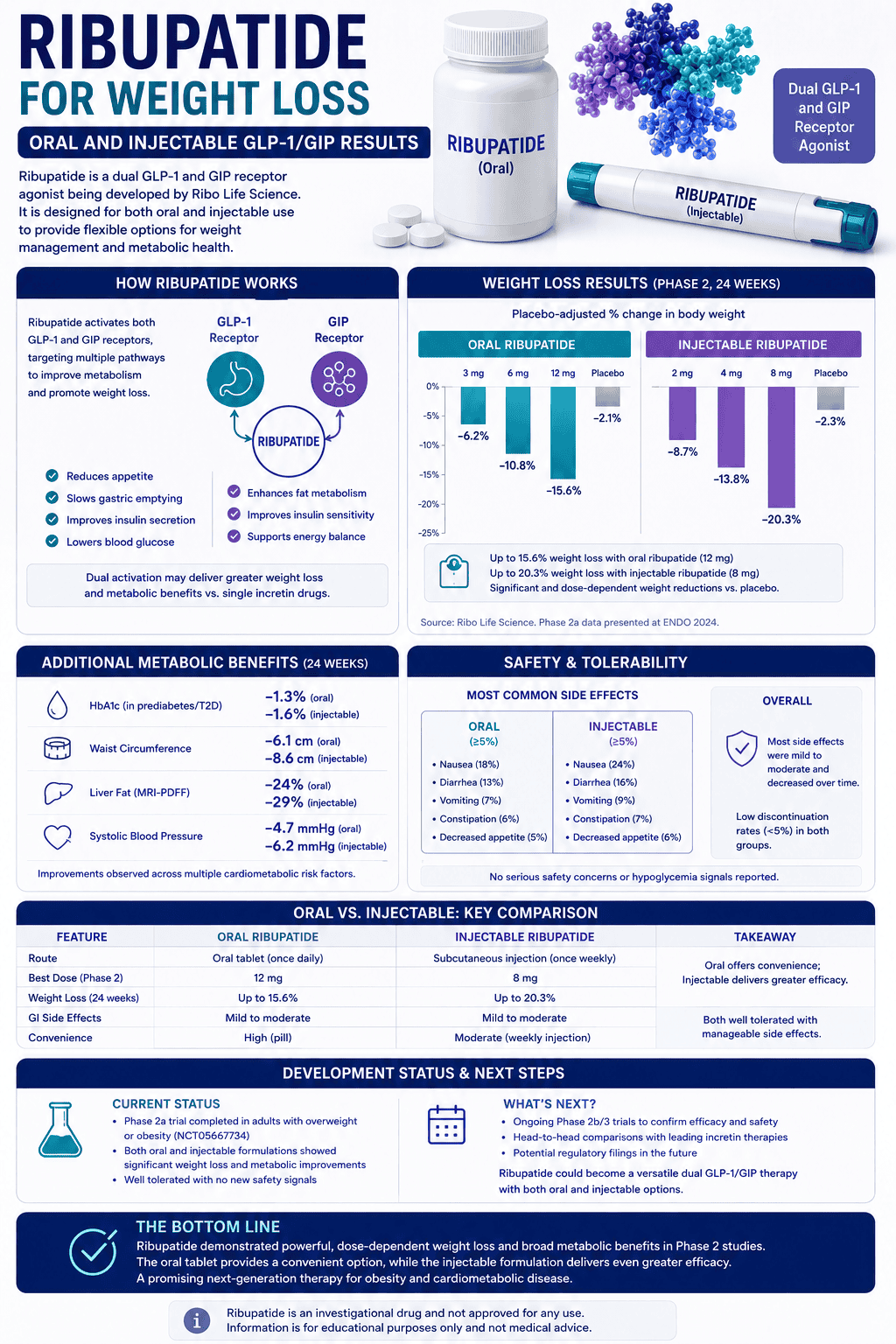
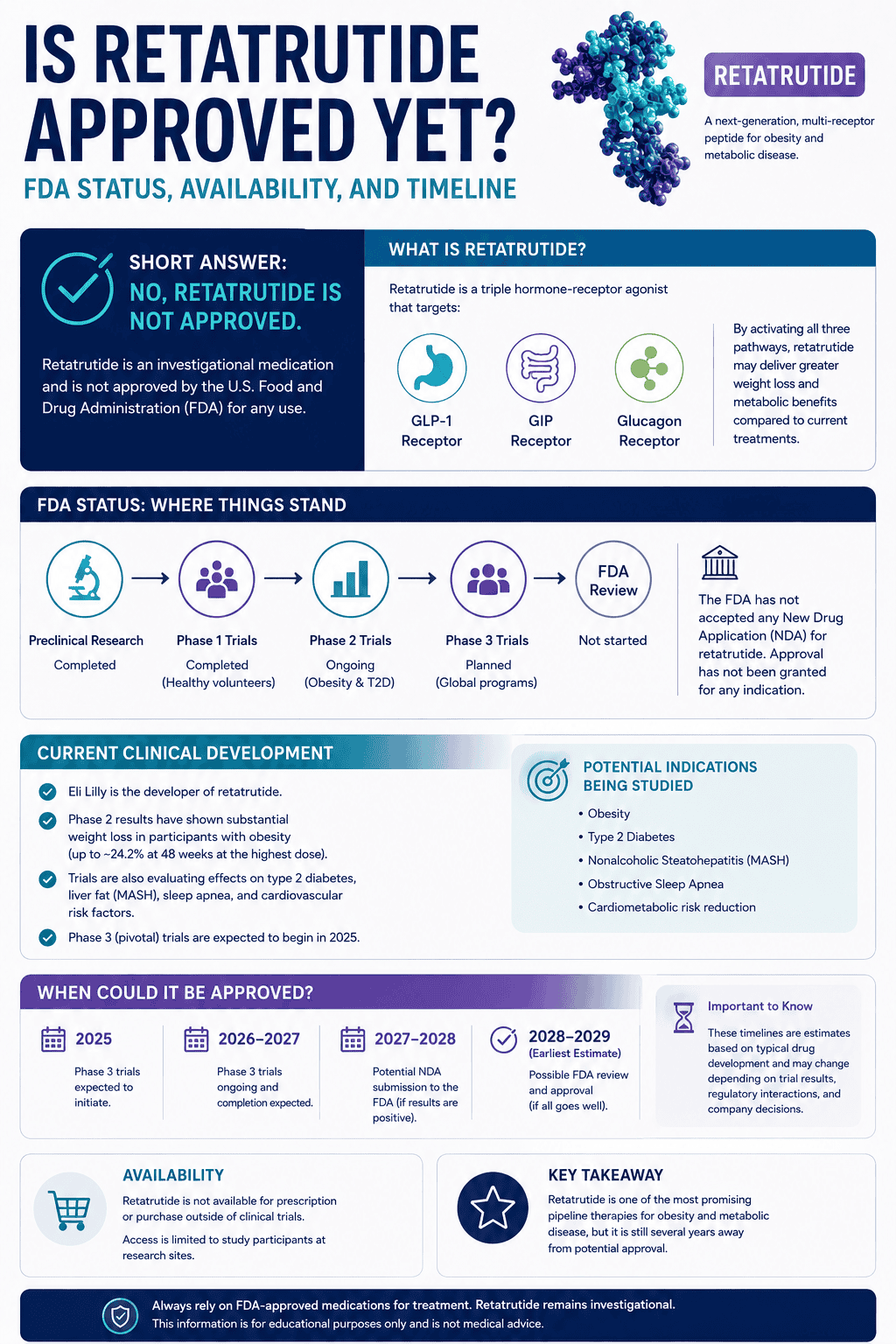
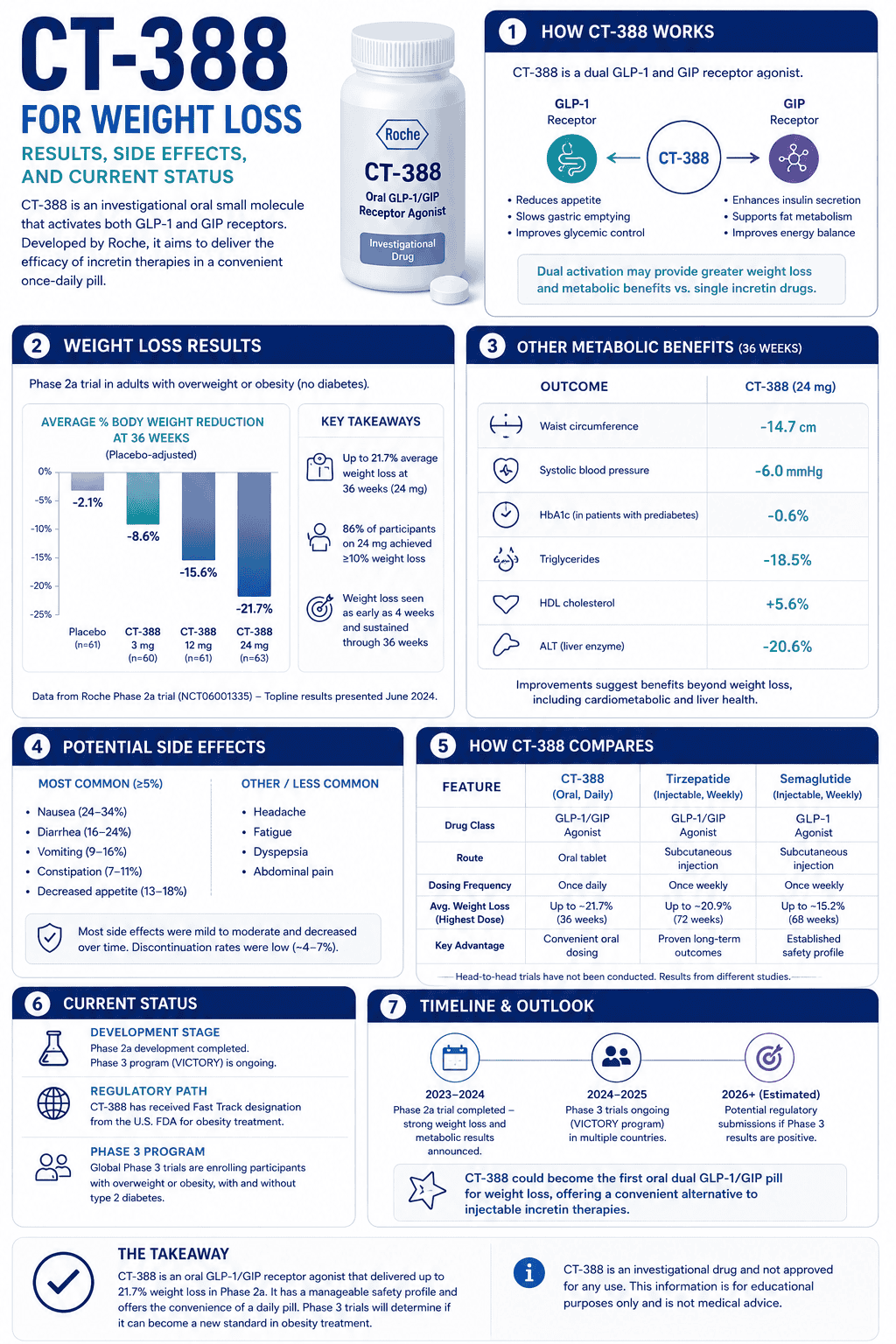
Direct answer: sodium and potassium do different jobs. Sodium mostly supports fluid volume and hydration stability (water outside cells). Potassium mostly supports cellular electrical balance and muscle output (water inside cells). Most people feel best when both are supported, but the “missing lever” depends on context.
If you feel “off” after sweating, heat, high water intake, or low-carb dieting, this page helps you pick the likely lever, test it cleanly, and avoid common mistakes.
What’s the difference between sodium and potassium?
They sit on opposite sides of cell membranes and drive fluid distribution and electrical signaling. Sodium is the main extracellular electrolyte (volume stability). Potassium is the main intracellular electrolyte (cellular electrical stability and muscle performance).
Do I need sodium or potassium?
Start with the dominant signal and the context that triggers it. If the trigger is heat/sweat + lots of water, sodium is often the first lever. If the trigger is weakness/cramps + low potassium foods, potassium is often the first lever (usually diet-first).
| Your dominant signal | Most likely lever | Best first move | Common mistake |
|---|---|---|---|
| Dizziness on standing, headache after water, worse in heat | Sodium | Pair sodium with fluids; test in the same heat/workout context | More plain water |
| Heavy legs, weakness, early fatigue, cramps with low fruit/veg | Potassium (diet-first) | Increase dietary potassium; check meds first | High-dose supplements without context |
| Symptoms fluctuate with heat, water, and training | Balance issue | Clean test one lever, then add the second if needed | Stacking everything at once |
| New palpitations or severe weakness | Medical evaluation | Get guidance; don’t self-treat with electrolytes | DIY potassium experiments |
- Kidney disease or reduced eGFR: potassium supplementation can be dangerous; sodium may also be restricted.
- ACE inhibitors/ARBs or potassium-sparing diuretics: increase hyperkalemia risk.
- Heart failure or clinician-directed sodium restriction: do not increase sodium without guidance.
- Severe hypertension or sodium-sensitive BP: context changes the sodium strategy.
- Vomiting/diarrhea/heat illness: higher stakes; treat hydration as medical when severe.
Signs you need more sodium
Sodium problems look like volume instability, especially in heat/sweat contexts or when water intake is high. Sodium is also the primary electrolyte lost in sweat.
- Dizziness/lightheadedness on standing
- Headaches after sweating or after lots of water
- Frequent urination without hydration relief
- Heat intolerance and “washed out” feeling after workouts
Signs you need more potassium
Potassium problems often look like electrical output issues: weakness, “heavy legs,” cramps with low output, and early fatigue. Potassium is best addressed food-first for most people.
- Weakness more than tension
- Heavy legs or early fatigue during activity
- Cramps with sweating and low fueling
- Constipation + fatigue can occur in low potassium states
Can drinking too much water mess up electrolytes?
It can—especially if sodium isn’t keeping up with water intake and sweat loss. That’s why “hydrating more” can sometimes worsen headaches, dizziness, and fatigue in heat or training contexts.
Electrolyte troubleshooting: how to tell it’s working
Electrolytes “work” when the trigger context becomes easier: less dizziness, fewer heat headaches, steadier output, fewer cramps. The biggest failure mode is stacking multiple changes and never learning the lever.
- Water-only hydration when sweating
- Using high-dose potassium supplements without context
- Ignoring food intake and relying on drinks only
- Judging on one day instead of repeatable triggers
- Pick one lever first: sodium (most common) or dietary potassium (food-first).
- Hold water intake stable (don’t “fix” hydration by doubling water mid-test).
- Test in a repeatable context (same workout time/heat exposure).
- Track 3 things: dizziness (0–10), headache (yes/no), output/energy (0–10).
- After day 7, add the second lever only if symptoms remain and safety context allows.
- Sodium win: less dizziness on standing; fewer heat/workout headaches within 2–7 days in the same context.
- Potassium (diet) win: fewer cramps/weakness episodes over 1–2 weeks (stable training).
- Balance win: symptoms become less volatile day-to-day.
- What not to expect: perfect hydration if illness, anemia, or medication effects are primary drivers.
- Confusion, fainting/near-fainting, chest pain, severe weakness
- Concerning palpitations or severe heat illness symptoms
- Known kidney disease or heart failure without clinician guidance
- Symptoms that escalate fast or feel dangerous
Go Deeper (VerifiedSupps Guides)
Final Takeaway
Sodium and potassium solve different problems. Sodium is the hydration-stability lever; potassium is the cellular-output lever. If you feel “off,” match the lever to the pattern, test one change at a time, and treat high-risk symptoms as medical—not DIY electrolyte projects.