Potassium Dosage Guide: Simple, Safe, Science-Backed
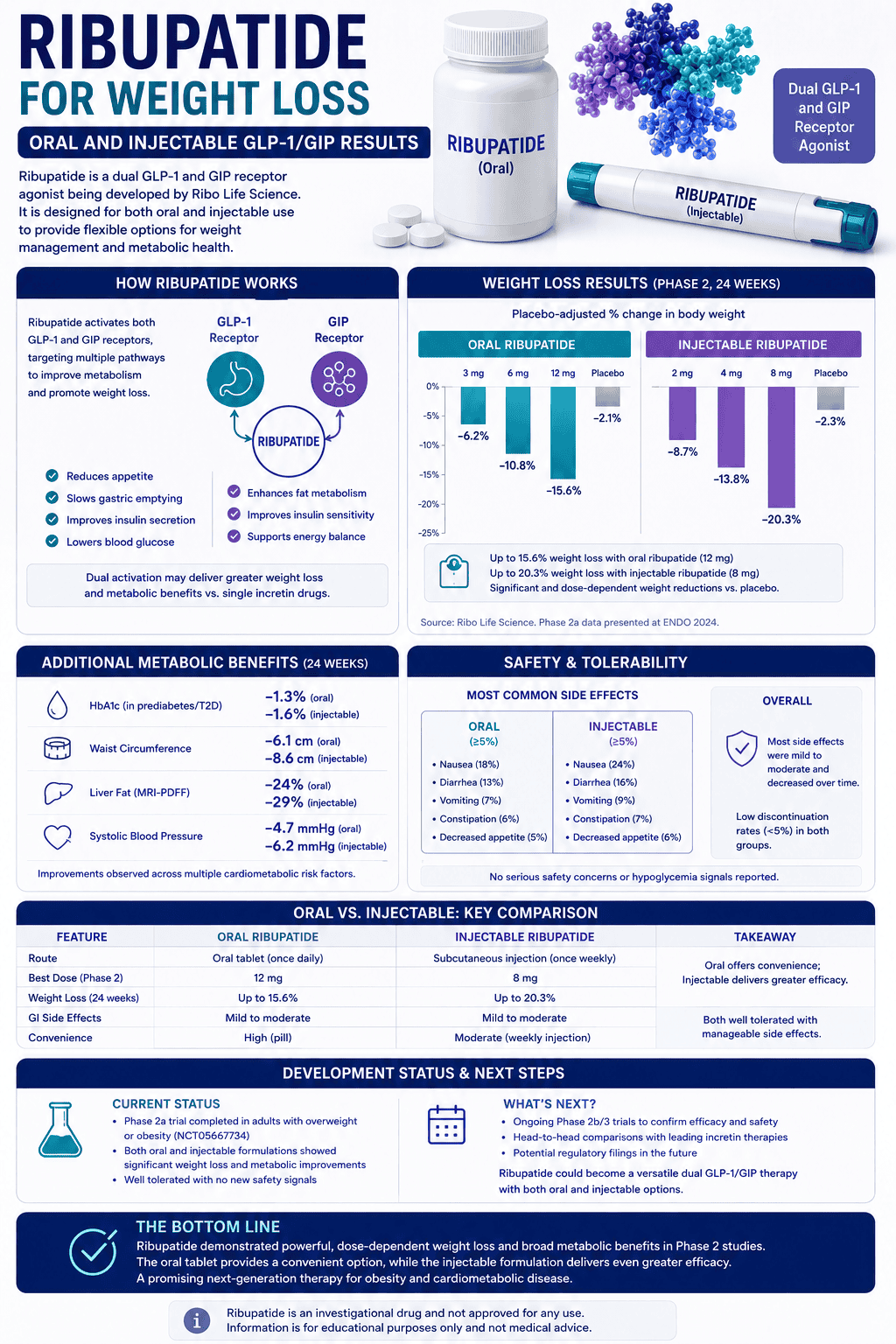
Direct answer: most potassium should come from food. Typical daily targets are roughly 2,600 mg (women) and 3,400 mg (men). Potassium supplements are usually low-dose (often 99 mg) because higher-dose potassium can be risky in the wrong medical context.
If you’re here because hydration feels inconsistent, legs feel heavy, cramps show up in heat, or workouts feel “flat,” potassium may be part of the picture—but it’s almost always a food-first lever and it works best with sodium + magnesium.
How much potassium do I need per day?
Most people should treat potassium as food-first. Common Adequate Intake targets are around 2,600 mg/day for women and 3,400 mg/day for men. Your needs shift with diet quality, sweat/heat exposure, and total electrolyte balance.
Cannibalization guardrail: this page is dosing + safety + testing; if you want the food list and meal ideas, use the “high potassium foods” guide.
- You’re low on fruits/vegetables and feel “flat” during workouts
- You get heavy legs or early fatigue, especially in heat
- Cramps show up during sweaty weeks (often sodium + potassium)
| Your intent | Most likely lever | Best next step (today) | Common mistake |
|---|---|---|---|
| Heavy legs / early fatigue | Dietary potassium | Add a potassium-heavy meal (potatoes/beans/greens) | Jumping to high-dose supplements |
| Cramps in heat | Sodium + potassium balance | Salted potatoes + fluids; repeatable test | Assuming magnesium alone |
| Hydration feels inconsistent | Often sodium first, then potassium | Test sodium support for 7 days; add potassium foods | More water without electrolytes |
| “I want supplements to replace food” | Not a great plan | Use supplements as small support; make food the base | Chasing numbers instead of habits |
- Kidney disease or reduced eGFR: potassium supplements can be dangerous.
- ACE inhibitors/ARBs or potassium-sparing diuretics (e.g., spironolactone): hyperkalemia risk.
- Known arrhythmias or concerning palpitations: clinician guidance first.
- Severe weakness, paralysis, confusion: urgent evaluation.
- Vomiting/diarrhea/heat illness: higher stakes; medical guidance if significant.
What is the best way to increase potassium?
Food is the best way to increase potassium because it delivers meaningful doses safely and consistently. The simplest high-yield pattern is: a potassium-rich starch (potatoes/beans) + greens + fruit.
Why are potassium supplements only 99 mg?
Many OTC potassium supplements are low-dose because higher-dose potassium can affect heart rhythm if used incorrectly, especially in people with kidney issues or potassium-retaining medications. The low dose is designed as gentle support—not replacement for food.
How much potassium is safe to take as a supplement?
For most people, potassium supplementation should stay conservative unless directed medically. Low-dose supplements are typically used to support hydration and recovery while food provides the bulk of intake. If you have kidney issues or potassium-retaining medications, supplementing can be unsafe.
When should I take potassium?
If you’re using low-dose potassium support, people commonly take it earlier in the day or around sweat/heat contexts. For most, timing is less important than consistent diet intake. If you’re testing potassium, keep timing stable to get clean feedback.
Who should not take potassium supplements?
People with kidney disease, those taking ACE inhibitors/ARBs, potassium-sparing diuretics, or those with certain heart rhythm disorders should not supplement potassium without clinician guidance. Food potassium is generally safer, but medical context still matters.
How to tell if potassium is working
Potassium “works” when cellular output improves: fewer heavy-leg days, less early fatigue, fewer cramps in heat—assuming sodium and magnesium aren’t the limiting factors. Most failures happen because the test isn’t clean or because potassium isn’t actually the bottleneck.
- Using low-dose pills to replace food potassium
- Ignoring sodium balance (water doesn’t “stick”)
- Changing caffeine, training, and electrolytes simultaneously
- Assuming cramps are potassium-only (often multi-factor)
- Inputs held constant: training schedule, caffeine, water intake, sodium intake pattern
- Duration: 7–14 days (diet-first), longer if your diet change is gradual
- 3 metrics: heavy legs (0–10), cramps frequency (count), workout output/energy (0–10)
- Stop conditions: concerning palpitations, severe weakness, chest pain, confusion, or any symptom that feels dangerous
- Within 7–14 days: fewer “heavy legs” days and less early fatigue (same training)
- Heat contexts: fewer cramps when sodium is also supported
- What not to expect: a dramatic “feel it now” effect from low-dose supplements
- If nothing changes: re-check sodium, magnesium, total calories, and heat stress
Selected Professional References
- NIH ODS: Potassium (Health Professional) — used for: intake targets, physiology, safety context
- MedlinePlus: Potassium blood test — used for: when labs clarify symptoms
- MedlinePlus: Low blood potassium (hypokalemia) — used for: warning signs and clinical context
- American Heart Association: Potassium and sodium balance — used for: balance framing (sodium vs potassium)
Go Deeper (VerifiedSupps Guides)
Final Takeaway
Potassium “dosage” is mostly a diet pattern: aim for food-first daily targets, and use low-dose supplements only as gentle support when appropriate. If hydration feels off, remember: sodium helps water stick, potassium helps hydration go inside cells, and magnesium supports stability. Test one lever at a time and keep it clean enough to learn.