Potassium Deficiency Signs: Simple, Science-Based Guide
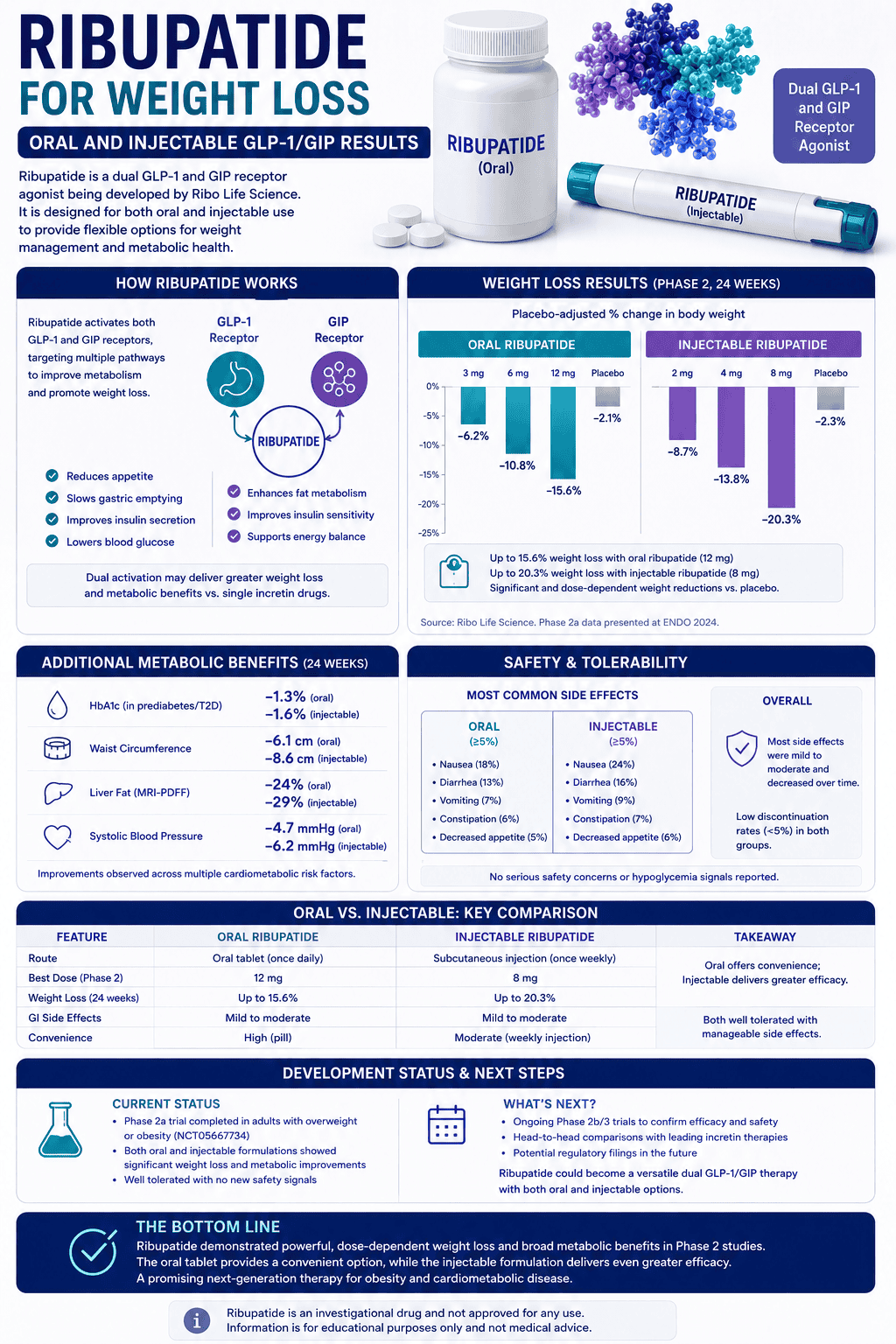
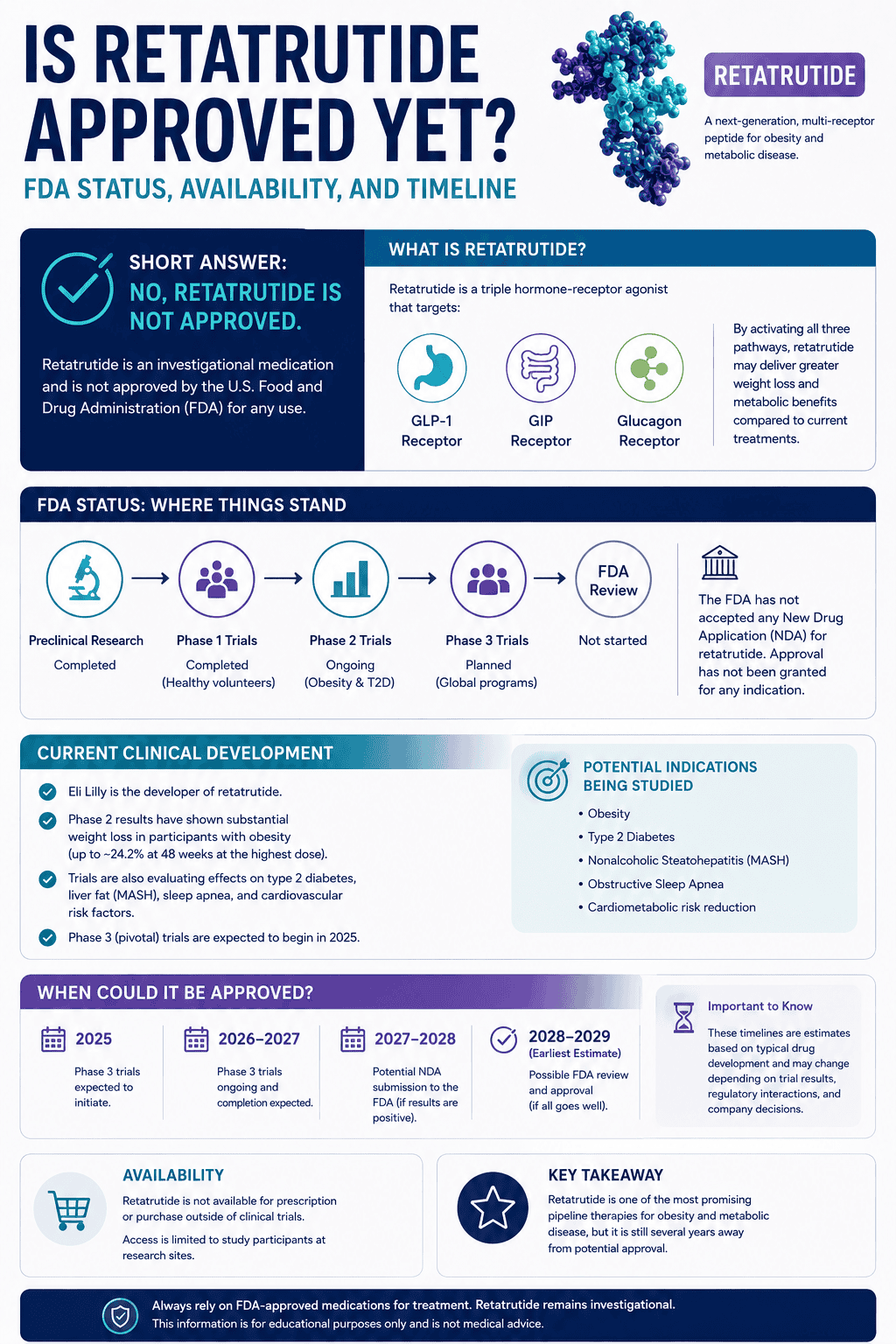
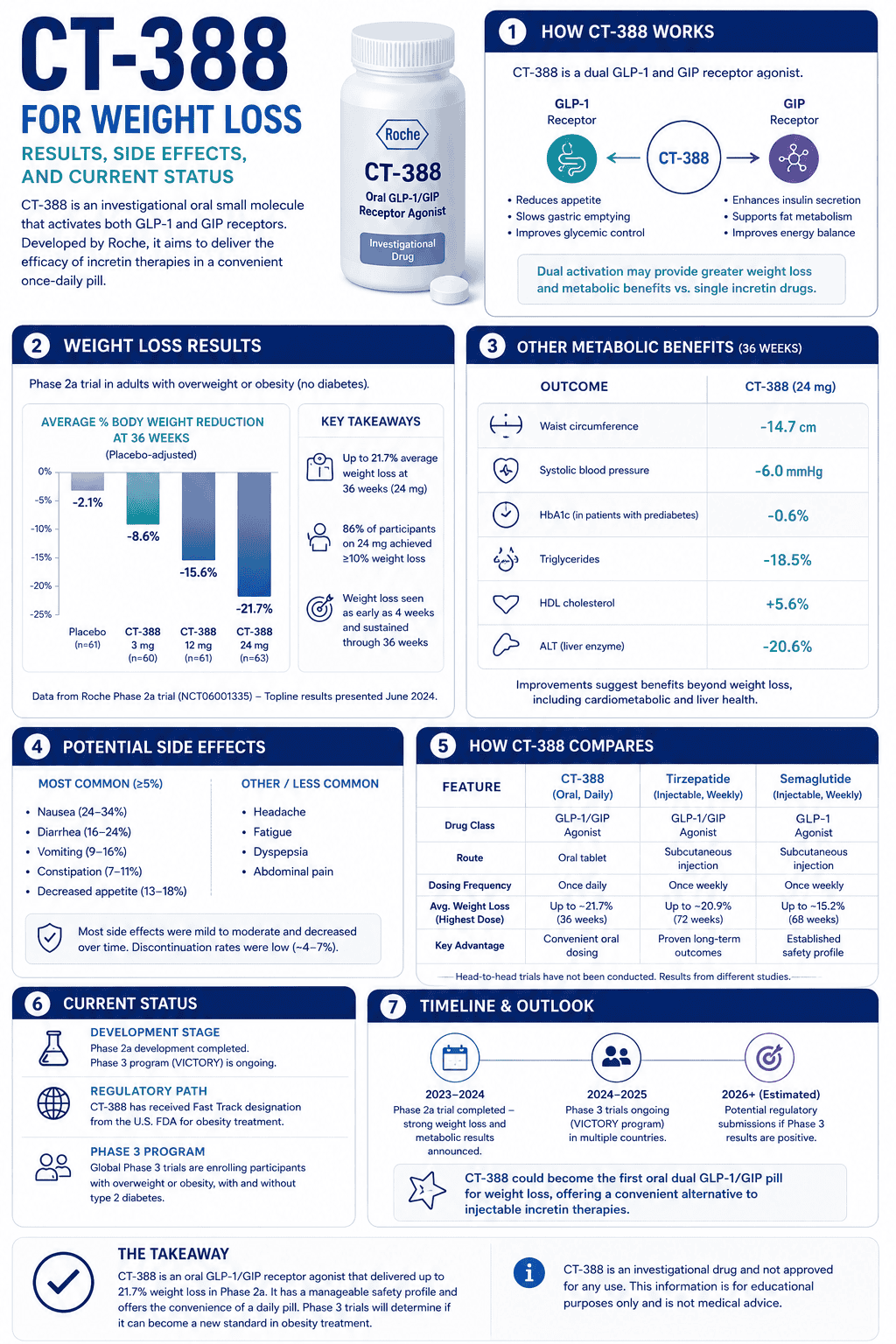
Direct answer: potassium runs your “inside-the-cell” electrical stability. When it’s low, the most common real-world patterns are heavy legs/weakness, early workout fatigue, cramps in heat, and hydration that feels inconsistent—especially if your diet is low in potassium-rich foods (potatoes, beans, greens, fruit) or your demand is high (sweat, heat, endurance).
This page owns one intent: spot the pattern and choose the safest next step. If symptoms are severe (fainting, chest pain, serious palpitations), treat it as medical first.
What are the signs of potassium deficiency?
Potassium deficiency most often shows up as reduced output: weakness, heavy legs, and earlier fatigue than usual—especially in heat or endurance. Symptoms tend to cluster rather than appear as one dramatic sign.
Cannibalization guardrail: this page is signs + how to test safely; if you want food lists and meal ideas, use the “high potassium foods” page.
- You’re low on potatoes/beans/greens/fruit most days
- You get heavy legs or early fatigue in warm weather
- Cramps appear mainly during sweating weeks (often sodium + potassium)
- Weakness/heavy legs (stairs feel harder, legs feel flat)
- Early fatigue (output drops sooner than expected)
- Cramps during heat/exercise (often not magnesium-only)
- Heat intolerance (you “overheat” faster)
- Constipation can co-occur (not diagnostic, but common)
- Heart awareness/palpitations can occur—treat persistent/new palpitations as medical
Is it low potassium or low sodium?
A useful split: sodium problems often feel like volume instability (dizziness, headaches after water, “water doesn’t stick”). Potassium problems often feel like cellular output issues (heavy legs, weakness, early fatigue). Overlap is common in heat and sweat.
| Your intent | Likely lever | Best next step (today) | Common mistake |
|---|---|---|---|
| Dizziness after lots of water | Sodium first | Salt a meal + fluids; repeat in same context | More water |
| Heavy legs / early fatigue | Potassium (diet-first) | Add potatoes/beans/greens today | Relying on 99 mg pills to “fix” diet |
| Cramps in heat | Balance (often sodium + potassium) | Salted potatoes + fluids | Assuming magnesium only |
| New palpitations | Medical evaluation | Get checked before DIY electrolytes | High-dose potassium experiments |
What causes low potassium?
The most common cause is simple: intake doesn’t match demand. Demand rises with heat, sweat, endurance training, low-carb phases, and inconsistent meals. Some medications and GI losses can also drop potassium and require medical supervision.
- Low potassium foods (low fruit/veg/beans/potatoes consistency)
- Heat + sweating + endurance training
- High water intake without balanced electrolytes
- GI losses (vomiting/diarrhea) — higher stakes
- Certain medications (diuretics, etc.) — clinician-guided
Can low potassium cause cramps or heavy legs?
Yes—especially the heavy legs / early fatigue pattern. Cramps are trickier: they can involve sodium loss, potassium, magnesium, fueling, and heat stress. If cramps happen mainly in heat or long cardio, balance is often the answer.
How do you fix low potassium fast?
For most people, the fastest safe fix is food-first potassium plus stable hydration: salted potatoes, beans/lentils, leafy greens, and fruit. Avoid jumping to high-dose potassium supplements unless medically directed.
- Salted potatoes (potassium + sodium balance)
- Beans/lentils (high potassium, high payoff)
- Greens + tomatoes (potassium-rich)
- Consistent fruit (e.g., bananas) as a repeatable habit
Who should not take potassium supplements?
Potassium from food is generally safer, but potassium supplements require context. If you have kidney disease or take potassium-retaining medications, supplementation can raise potassium too high.
- Kidney disease / reduced eGFR
- ACE inhibitors / ARBs
- Potassium-sparing diuretics (e.g., spironolactone)
- Known arrhythmias or persistent palpitations
- Severe dehydration/heat illness or major GI losses
How to tell if potassium is working
Potassium is working when your output stabilizes: fewer heavy-leg days, less early fatigue, fewer cramps in heat—assuming sodium and magnesium aren’t the limiting factors. Low-dose pills usually won’t feel dramatic; the signal is trend-based.
- Trying to “supplement” your way out of a low-potassium diet
- Ignoring sodium on sweat/heat days
- Changing caffeine, training volume, and electrolytes simultaneously
- Not tracking the right metric (output vs “feeling it”)
- Inputs held constant: training schedule, caffeine, water intake, salt/sodium pattern
- Duration: 7–14 days (diet-first)
- 3 metrics: heavy legs (0–10), cramps count, workout energy/output (0–10)
- Stop conditions: concerning palpitations, severe weakness, chest pain, confusion, fainting/near-fainting
- Within 7–14 days: fewer heavy-leg days and less early fatigue (same training)
- Heat contexts: fewer cramps when sodium is also supported
- What not to expect: a dramatic “feel it now” effect from low-dose supplements
- If nothing changes: re-check sodium, magnesium, total calories, sleep, and heat stress
Selected Professional References
Go Deeper (VerifiedSupps Guides)
Final Takeaway
If your pattern is heavy legs, early fatigue, and cramps in heat—especially with low potassium foods—potassium is worth checking. Start food-first for 7–14 days, keep hydration and salt stable, and judge by trends (output, cramps frequency, heat tolerance), not sensations.