Magnesium vs Potassium: What’s the Difference and Do You Need Both?
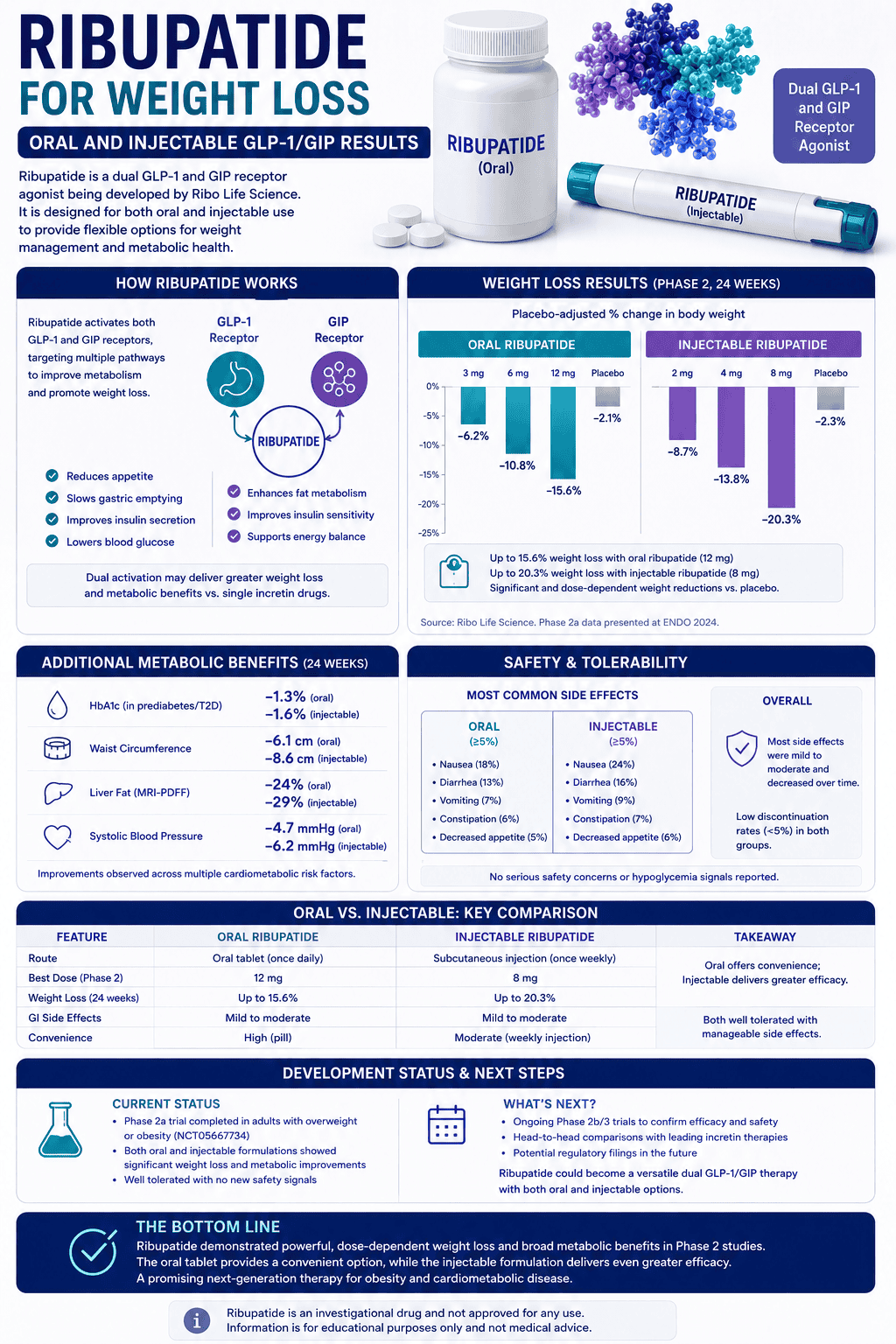
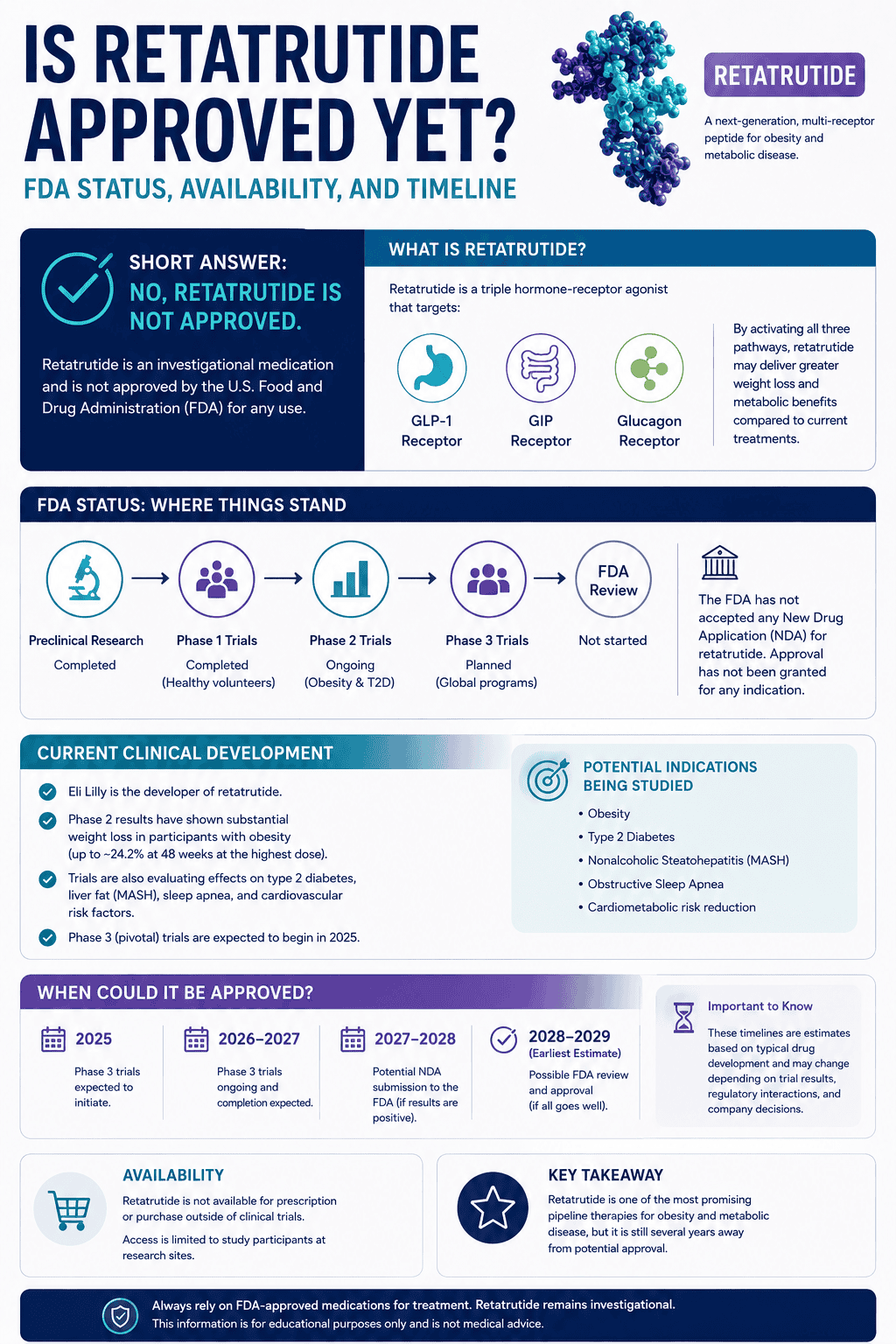
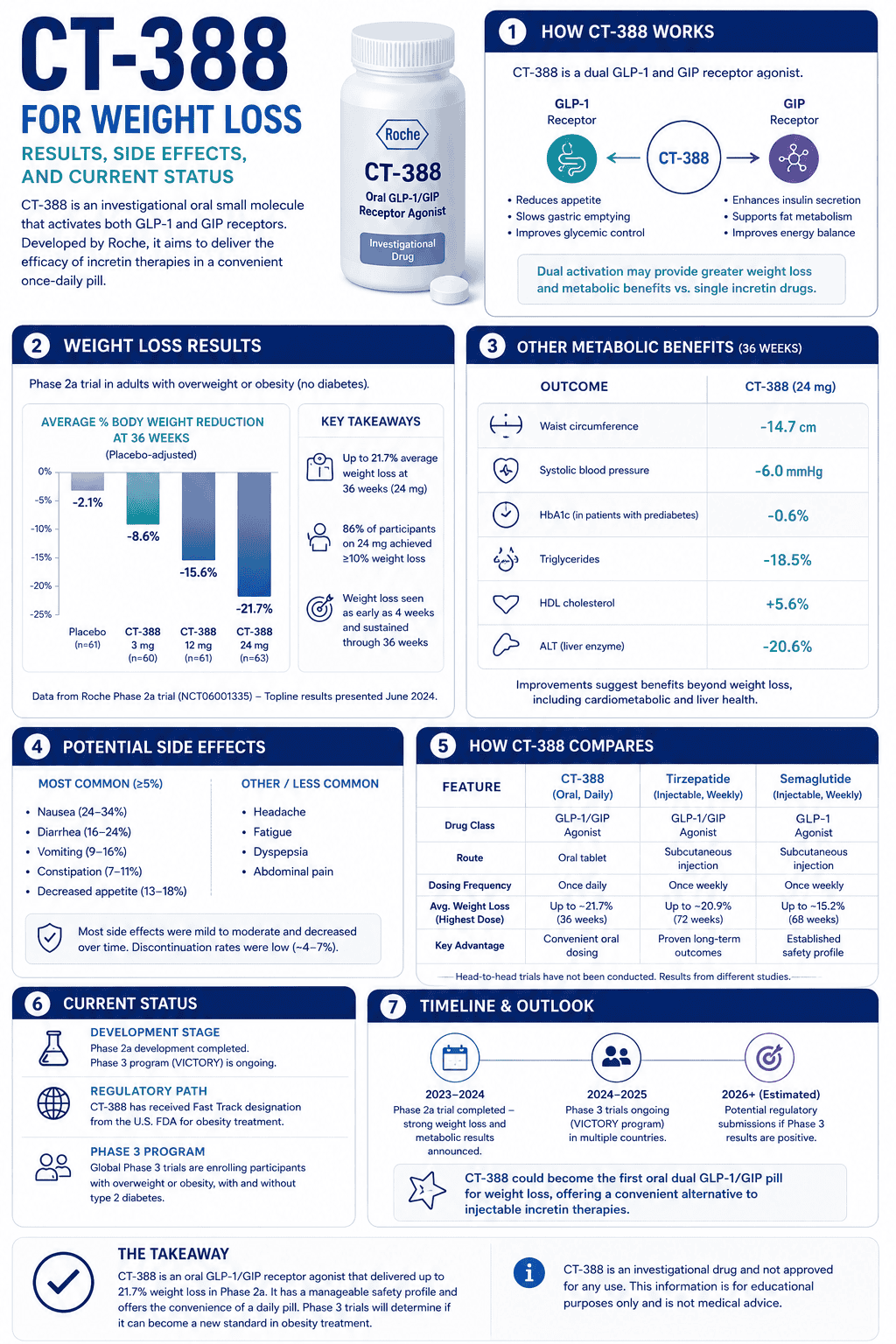
Direct answer: potassium is the main “inside-the-cell” electrolyte (electrical balance, muscle contraction, cellular hydration). magnesium is the “regulation and release” mineral (relaxation threshold, energy reactions, nervous-system stability) and it can affect how well cells handle potassium.
Intent/scope: this page is a pattern-to-lever comparison (what low magnesium vs low potassium tends to feel like, and what to do first). It is not a diagnosis guide for chest pain/persistent palpitations or severe weakness—those need medical evaluation.
What is the difference between magnesium and potassium?
Potassium is primarily about electrical balance and contraction inside cells. Magnesium is primarily about regulation and relaxation—and it supports many reactions that keep nerves and muscles stable.
- Potassium: maintains intracellular fluid volume and electrochemical gradients (muscle contraction and nerve firing)
- Magnesium: supports neuromuscular stability and relaxation threshold
- Interaction: low magnesium can make potassium regulation harder in some contexts
| If you feel… | Often points to… | Best next step (today) | Common mistake |
|---|---|---|---|
| Twitches, jaw/neck tension, tight calves, poor wind-down | Magnesium pattern | Start a gentle magnesium routine for 10–14 days | Using a gut-active form and quitting |
| Weakness/heavy legs, “flat” output, heat intolerance | Potassium foods + hydration balance | Add potatoes/beans/greens daily for 7 days | Relying on low-dose pills to replace food |
| Cramps + stress + poor sleep + inconsistent hydration | Both may matter | Potassium foods daily + magnesium consistency | Changing three variables at once |
| Concerning palpitations, chest pain, fainting | Could be electrolytes or many other causes | Medical evaluation first | Self-treating severe symptoms |
- Kidney disease or reduced kidney function (supplement caution)
- ACE inhibitors/ARBs or potassium-sparing diuretics (higher potassium risk)
- Heart failure/arrhythmias or clinician-directed electrolyte limits
- New/persistent palpitations, chest pain, fainting/near-fainting
- Persistent vomiting/diarrhea or suspected heat illness
Do you need magnesium and potassium together?
Often, yes—because they operate in the same neuromuscular system. Many people get enough potassium only when they eat potassium-rich foods consistently. Many people get magnesium benefits only when they take it consistently (and tolerate the form).
- Potassium: potatoes, beans/lentils, spinach/greens, avocado, bananas, yogurt
- Magnesium: consistent routine (often glycinate for calm/sleep)
- Hydration: keep water intake stable so you can read the signal
What are signs of low magnesium vs low potassium?
They overlap, but the “feel” often differs. Magnesium tends to be tension/twitch/sleep/stress. Potassium tends to be weakness/heavy legs/low output—especially with heat or endurance.
- Twitches, tight jaw/neck, restless wind-down
- Night cramps with light sleep
- Stress sensitivity or irritability
- “Wired but tired” fatigue
- Weakness, heavy legs, low endurance output
- Heat intolerance or “flat” workouts
- Low potassium foods most days
- Occasional rhythm awareness (evaluate if concerning)
How much magnesium and potassium do you need per day?
Potassium targets are generally food-first (commonly cited AIs are higher than most people realize). Magnesium supplement routines often sit in the low-hundreds of elemental milligrams depending on the goal and tolerance.
- Potassium: commonly cited AIs are ~2,600 mg/day (women) and ~3,400 mg/day (men), mostly from food
- Magnesium: many people trial 100–350 mg/day elemental from supplements (adjust to tolerance)
- Reminder: potassium supplements are not “free dosing” for everyone—food-first is usually safest
Why am I still feeling off after taking magnesium or eating more potassium?
Most misses are: inconsistent routine, a missing electrolyte (often sodium), sleep debt, training spikes, or a medical/medication factor. Treat this like a clean test, not a pile-on stack.
- Changing water intake, caffeine, and training volume simultaneously
- Trying potassium pills instead of potassium foods
- Using a gut-active magnesium form and quitting
- Ignoring sweat/heat patterns (sodium can be the missing lever)
- Fainting/near-fainting, confusion, severe weakness
- Chest pain, new/persistent palpitations, shortness of breath
- Persistent vomiting/diarrhea or suspected heat illness
- Kidney disease or electrolyte-altering meds with worsening symptoms
- Severe dehydration or inability to keep fluids down
- Inputs: keep water intake, caffeine timing, and training schedule stable
- Duration: 7 days for potassium foods; 10–14 days for magnesium routine
- 3 metrics: energy stability (0–10), cramps/twitches count, sleep quality (0–10)
- Stop conditions: severe palpitations, chest pain, confusion, fainting/near-fainting
- Potassium foods: less heavy-leg fatigue and steadier output within 7–14 days
- Magnesium routine: fewer twitches/tension nights over 10–14 days
- What not to expect: a dramatic “kick”
- If no change: reassess sodium/hydration, sleep debt, illness, and medication effects
Selected Professional References
Go Deeper (VerifiedSupps Guides)
Final Takeaway
Potassium helps the system fire; magnesium helps it regulate and release. If you’re choosing between them, use the symptom pattern: heavy legs/low output → potassium foods; twitchy/tight/wired-but-tired → magnesium routine. Many people feel best when both are supported consistently (food-first potassium + gentle magnesium).