By VerifiedSupps Editorial Team
Are Peptides Safe? What You Need to Know Before Using Them
Sometimes. But “peptides” is too broad to answer with one yes-or-no. An FDA-approved peptide prescribed for a real medical reason is a very different safety situation from a compounded injectable, and both are very different from something sold online as a “research peptide.”
That is the part most people miss. The biggest safety question is not whether a product is called a peptide. It is which peptide it is, where it came from, how it is made, what dose and route are being used, and whether anyone legitimate is actually supervising it.
This page is for the broad peptide safety decision: approved peptide drugs, compounded peptides, and gray-market “research” peptides are separated clearly so you can judge risk more realistically.
Key terms: peptide safety, research peptides, compounded peptides, peptide injections, immunogenicity, contamination, dosing errors, online peptide risk
Quick Take
The safest default is this: approved prescription peptide first, medically justified compounded peptide second, and online “research” peptide last. If the source is vague, the concentration is unclear, or the product is sold with “not for human consumption” language while still giving dosing instructions, that is not a reassuring gray area. It is a warning sign.
TL;DR decision
Some peptide medicines are legitimate and can be reasonably safe when prescribed and monitored. But if you are considering a compounded peptide without a strong medical reason, or a “research peptide” bought online, the risk picture gets worse fast.
Evidence standard: human trials, dose ranges, guideline-level sources when available
Who this is for: anyone thinking about using a peptide for weight loss, recovery, anti-aging, performance, libido, or a medical condition and trying to judge risk before starting
Who this is not for: anyone looking for black-market sourcing advice, dosing for illegal use, or reassurance that a vague internet peptide is “probably fine”
Reviewed by: VerifiedSupps Editorial Team
Last reviewed: April 15, 2026
Parent Hub
VerifiedSupps Articles
Browse the wider evidence-based library if you want safer, more established options before drifting toward high-risk gray-market products.
Quick decision table: which peptide situation are you actually in?
This is the fastest way to avoid a bad shortcut. Most peptide safety questions become much clearer once you separate regulated products from everything else.
| What you are considering | Practical safety answer | Biggest risk | Best next step |
|---|---|---|---|
| An FDA-approved peptide prescribed for a real diagnosis | Usually the safer lane | Normal product-specific side effects, dosing, and monitoring still matter | Use the actual prescribing information and clinician follow-up |
| A compounded peptide because an approved option does not meet a real patient need | Higher risk, case by case | No FDA premarket review for safety, effectiveness, or quality | Verify the medical reason, product source, concentration, and dosing plan |
| A peptide sold online as “research only” or “not for human consumption” | Do not treat this as safe | Unknown quality, legality, strength, and contamination risk | Do not buy it for self-use |
| A compounded injectable from a clinic or telehealth service with vials and syringe instructions | Use extra caution | Dose-conversion errors, varying concentrations, and injection mistakes | Make sure the dose, units, syringe, and concentration all make sense before first use |
Best next step (today): Before you think about “which peptide,” decide which category you are actually dealing with: approved, compounded, or research-market.
Are peptides safe?
Some are. Some clearly are not. And some sit in a much riskier middle ground than marketing makes them look.
The clean answer is that peptides are not one safety category. Approved peptide drugs can be reasonable to use under normal prescribing and monitoring. But once you move into compounded products, custom mixtures, or online “research” peptides, the safety conversation stops being mostly about pharmacology and starts becoming heavily about product quality, concentration, contamination, formulation, and whether the product should have been used by a consumer in the first place.
Mechanism
- The peptide sequence and target determine what the product does biologically, which is why different peptides can have completely different side-effect profiles.
- Dose, route, and formulation change exposure. A peptide in a standardized approved product is not the same risk as one drawn from a vial with unclear concentration.
- Manufacturing matters. Regulators specifically flag peptide-related impurities, aggregation, and immunogenicity as meaningful safety issues for peptide products.
What would change my recommendation: if you are talking about an approved prescription peptide from a licensed clinician and pharmacy, I become much more comfortable. If you are talking about a research peptide site, an influencer link, or a vague compounded anti-aging stack, the answer shifts hard toward caution or no.
What makes one peptide safer than another?
The biggest safety divider is not “medical peptide” versus “fitness peptide.” It is regulated product versus poorly controlled product.
That is why the same broad word can hide very different realities. A standardized approved product comes with reviewed labeling, known concentration, fixed instructions, and a real supply chain. A compounded peptide comes with less certainty because FDA does not review it for safety, effectiveness, or quality before marketing. A research-market peptide adds another layer of uncertainty because even the basic assumptions about origin, labeling, concentration, and sterility may no longer deserve trust.
- Source: licensed pharmacy and real prescription beats anonymous site and vague checkout flow.
- Formulation: prefilled, fixed-dose products are easier to use safely than variable-concentration vials.
- Need: a real diagnosis and plan lowers the odds that you are solving the wrong problem with the wrong product.
- Monitoring: the more complex the product, the less sense it makes to use without clear follow-up.
Are research peptides or online peptides safe to use?
As a practical rule, no. The safest assumption is that an online peptide sold to consumers as “research only” is not a trustworthy self-use product.
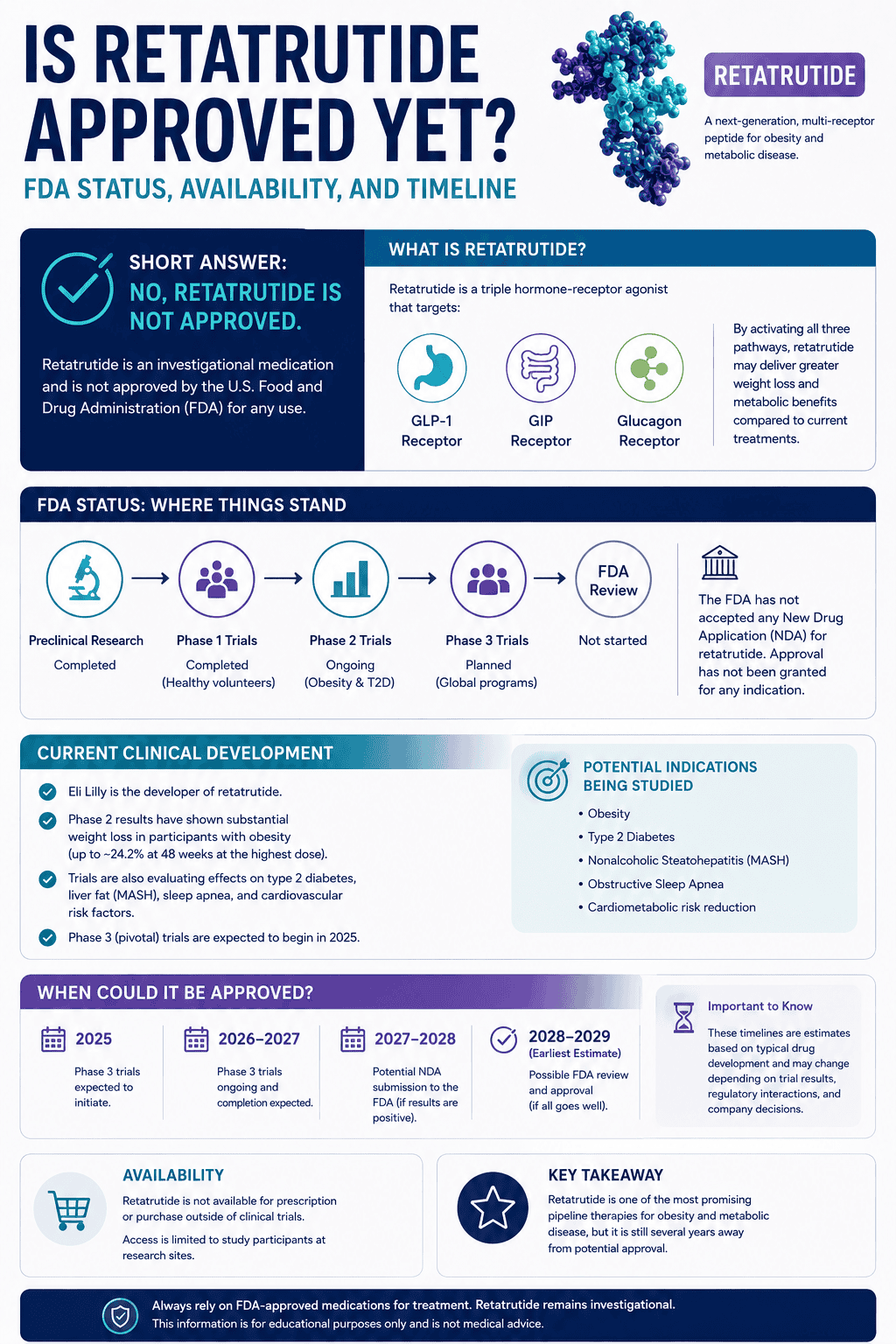
FDA has specifically warned about drugs containing semaglutide, tirzepatide, and retatrutide being sold online as “for research purposes” or “not for human consumption” even while being marketed to real people with dosing instructions. The agency says these products are of unknown quality and may be harmful. FDA has also issued recent warning letters to multiple peptide-selling websites offering products such as tirzepatide, retatrutide, cagrilintide, and other peptide products as unapproved new drugs.
This problem is bigger than GLP-1 products. FDA’s peptide compounding risk list includes several popular names seen in fitness, recovery, or anti-aging circles. For example, FDA says BPC-157 has no or only limited safety-related information for the proposed routes of administration, CJC-1295 has limited clinical data with reported serious adverse events, and Melanotan II has published case reports discussing serious adverse events.
If a site is willing to hide behind “not for human consumption” while obviously targeting human self-use, that is not a trust signal. It is one of the clearest reasons to step back.
Does dose, route, and formulation change peptide risk?
Yes, a lot. This is where people get hurt even when the ingredient name looks familiar.
FDA’s semaglutide warnings are a good example of the broader problem. With compounded injectable semaglutide, the agency reported adverse events, some requiring hospitalization, tied to dosing errors. Problems included patients measuring the wrong amount from a vial, confusion between milligrams, milliliters, and “units,” different product concentrations, and health care providers miscalculating doses.
That is why route and packaging matter. A fixed-dose approved pen is one kind of safety environment. A variable-concentration vial plus syringe math is another. Even before you get to the biology of the peptide itself, the practical chance of using the product incorrectly can be much higher.
This is also one reason injectable peptides deserve more respect than a capsule from the supplement aisle. Sterility, dilution, storage, measurement, and technique are not minor details. They are part of the safety profile.
What should you do before using a peptide for the first time?
Treat the first dose like a safety decision, not a biohacking milestone. If you cannot clearly answer what the product is, why you are using it, how it should be dosed, and who is accountable for problems, you are not ready to start.
Common mistakes
- Treating all peptides as one category instead of separating approved, compounded, and research-market products.
- Buying a “research” peptide and assuming a certificate, influencer, or forum thread makes it safe.
- Starting with a vial and syringe without being crystal clear on concentration, units, and exact dose.
- Running multiple new peptides or add-on ingredients at once, which makes side effects and benefit impossible to interpret.
Clean test protocol
| Inputs | Exact peptide name, exact concentration, route, source, storage instructions, prescribing clinician or pharmacy details if applicable, and a clear medical or functional reason for use |
|---|---|
| Duration | Do the safety check before the first dose, then reassess after the first few doses and at every dose change. Do not improvise the plan in real time. |
| 3 metrics | Can you dose it correctly without confusion, are side effects tolerable, and is there a clear benefit tied to the reason you started it |
| Stop conditions | Unclear source, unclear concentration, rash, swelling, severe nausea or vomiting, fainting, chest pain, palpitations, spreading injection-site redness, fever, or any reaction that makes you doubt the product or your dosing |
How to tell it’s working
“I felt something” is not enough. The benefit should match the reason you took it in the first place, and it should not come at the cost of confusing side effects, dose uncertainty, or obvious product concerns.
Red flags / seek care
Seek medical care right away for trouble breathing, severe allergic-type reactions, fainting, chest pain, severe palpitations, severe dehydration, severe abdominal pain, infection signs after injection, or a major reaction after what might have been the wrong dose.
When should you avoid peptides and talk to a clinician first?
Your threshold for self-experimenting should be much higher if any part of the situation is unclear. That includes unclear diagnosis, unclear source, unclear dose, unclear route, or unclear instructions.
Be even more careful if you are inexperienced with self-injections, already take multiple prescription medications, or are being offered a compounded peptide even though an approved product already exists for the job. FDA’s position is that compounded drugs should be used only when a patient’s needs cannot be met by an available FDA-approved drug.
This is also where the purpose matters. The weaker the medical reason, the less sense it makes to accept higher uncertainty. If the use case is mostly cosmetic, anti-aging, recovery optimization, or curiosity, that is usually not the place to lower your standards for product quality and oversight.
And if the product is being sold as “research only,” you do not need a deeper risk-benefit debate. You already have your answer.
Selected Professional References
These are the key official sources behind the approved-versus-compounded-versus-research safety split used throughout this page.
Understanding the Risks of Compounded Drugs
The cleanest official explanation of why compounded drugs carry more uncertainty than approved products.
Used for: the approved-versus-compounded safety split
Consumer and Health Care Professional Information
Important for contamination, wrong-strength, purity, and serious injury risk from poor compounding practices.
Used for: contamination and quality-risk framing
FDA’s Concerns with Unapproved GLP-1 Drugs Used for Weight Loss
Directly addresses online peptide drugs sold as “for research purposes” or “not for human consumption.”
Used for: research-peptide warning language
Certain Bulk Drug Substances That May Present Significant Safety Risks
One of the most useful official lists for names like BPC-157, CJC-1295, ipamorelin, semax, and Melanotan II.
Used for: popular peptide examples and regulator concern
Dosing Errors with Compounded Injectable Semaglutide
Very useful for understanding how packaging, syringe math, and concentration confusion become real safety problems.
Used for: dose-conversion and self-injection risk
Immunogenicity Assessments in Peptides: Progress and Remaining Challenges
A useful reality check that peptide drugs are an established class, but still require careful impurity and immune-risk assessment.
Used for: “some peptides are real medicines” plus immunogenicity context
Guidance for Industry: Synthetic Peptides
Shows why peptide-related impurities and immunogenicity are treated as real regulatory safety issues.
Used for: manufacturing quality and impurity risk
Guideline on the Development and Manufacture of Synthetic Peptides
Helps show that peptide quality control is specialized, not a trivial extension of regular supplement manufacturing.
Used for: why peptide manufacturing complexity matters
FDA Green List for Illegal Imported GLP-1 Ingredients
Useful if your concern is overseas APIs, unofficial sourcing, and the false comfort of imported “pharma grade” claims.
Used for: source-quality and import-risk context
Go Deeper (VerifiedSupps Guides)
These are better next reads if your real goal is not “peptides,” but recovery, stress support, or smarter supplement decisions with lower uncertainty.
How to Choose Supplements Without Guesswork
Best next step if you want a more disciplined framework before jumping to high-risk products.
Muscle Growth + Recovery Stack
Useful if your real interest in peptides is performance or recovery and you want a lower-risk evidence-based route first.
Best Supplements for Stress Relief
A better path if the goal is feeling better, not experimenting with uncertain injectable products.
How Much Protein Do You Actually Need?
Helpful when the real goal is body composition or recovery and basic fundamentals still are not nailed down.
Final Takeaway
Peptides are not automatically safe, and they are not automatically dangerous. The cleanest rule is to separate the category into three buckets: approved prescription peptide, medically justified compounded peptide, and online research peptide. The farther you move away from approved products and clear medical oversight, the more the risk shifts from normal side effects toward quality, contamination, dose confusion, and basic trust problems. If the source or instructions feel vague, that is the signal to slow down, not push forward.
FAQ
Are all peptides experimental?
No. Some peptide drugs are legitimate approved prescription medicines. The safety problem starts when people treat approved peptides, compounded peptides, and online research peptides as if they are the same thing.
Is an FDA-approved peptide safer than a research peptide?
Usually yes. An approved peptide comes with reviewed labeling, known concentration, and a real supply chain. A research peptide sold online does not offer the same assurance.
Are compounded peptides the same as approved peptides?
No. Compounded drugs are not FDA-approved, and FDA does not review their safety, effectiveness, or quality before marketing.
Are peptides sold “for research only” safe if people still use them?
That label is not a safety shield. FDA has specifically warned consumers not to buy products sold that way when they are clearly being marketed for human use.
Why are injectable peptides riskier than regular supplements?
Injection adds sterility, measurement, concentration, storage, and technique issues. With variable-concentration vials, dosing errors can become part of the risk.
Are BPC-157 or CJC-1295 automatically safe because they are popular?
No. Popularity is not proof of safety. FDA has flagged several popular peptides for limited safety data, immunogenicity concerns, or reported serious adverse events.
Can peptides interact with prescription drugs?
Yes, depending on the peptide. Drug interactions are not a made-up concern here, which is another reason peptide-specific review matters.
What should I verify before the first dose?
You should know the exact peptide, exact concentration, exact route, exact dose, exact source, and what problem it is supposed to solve. If any of those are fuzzy, do not start.
When should I stop immediately and seek help?
Stop and seek care for severe allergic symptoms, fainting, chest pain, severe palpitations, severe vomiting or dehydration, infection signs after injection, or a major reaction after a suspected dosing error.
Can peptides replace diagnosis or prescription treatment?
No. A peptide is not a shortcut around figuring out what is actually wrong, and gray-market peptides are not substitutes for medical evaluation or approved treatment.
VerifiedSupps Medical Disclaimer
This content is for educational purposes only and is not medical advice. “Peptides” include both approved prescription drugs and unapproved products sold through compounding or research markets, so safety cannot be judged by category name alone. Do not use a peptide product as a substitute for diagnosis, clinician review, or approved treatment. Be especially cautious with injectable products, compounded vials, unclear concentrations, and anything sold as “research only” while being marketed for human use. Seek urgent medical care for allergic reactions, chest pain, fainting, severe vomiting or dehydration, severe palpitations, or infection signs after injection.